I am a veterinarian with 22 years of experience in feline medicine. I am a member of the American Veterinary Medical Association (AVMA), American Veterinary Society for Animal Behavior, International Veterinary Academy of Pain Management, Veterinary, Society for Veterinary Medical Ethics, and Humane Society Veterinary Medical Association. I have been concerned about declawing since my senior year of vet school. To me, declawing was obviously a wholly barbaric, horrible thing to do to a cat. Despite my misgivings, as a new graduate I practiced in a feline-only clinic and performed hundreds of declaws. In only one case was declawing medically necessary for the cat. I made it my mission to research everything known about declawing. This paper sums up my research on the pain associated with declawing. When the evidence is taken as a whole, declawing is clearly an egregious form of animal cruelty. If you have any doubts, please read on.
Dr Jean Hofve, DVM
The Pain of Declawing

Cats are notorious for hiding pain. They are incredibly stoic. Many studies have sought for signs or ways to assess pain in cats, looking at everything from blood cortisol levels (high cortisol indicates stress), blood pressure, posture, and behavior. None have proven consistently accurate.[i] [ii] [iii] [iv]
This obviously works to the disadvantage of cats. When I was a senior in surgery rotation in veterinary school, a fellow student asked, “Why don’t we declaw dogs?” The answer? “Because they scream.”
Yes, dogs are much more demonstrative of pain. They may not always scream, but they certainly whine, growl, and otherwise communicate their state of body and mind. Cats don’t scream. It’s not easy to know how much pain they’re in. Veterinarians are not trained how to recognize feline pain; lay people are much less able to do so.
If a declawed cat is painful on both paws, it won’t limp. It will walk a little differently, but that may not be noticeable. If that strange gait persists, human family members will come to see it as normal. Even if the cat does limp once in a while, is that something that will be mentioned in the cat’s next 15-minute annual exam visit?
Many veterinarians, particularly those who have testified against proposed declaw bans, claim that they declaw with excellent surgical technique and perfect multi-modal pain management. That’s great—but it’s not standard. It’s not mandatory. Many veterinarians provide what is today considered adequate pain management, despite its deficiencies, but this is far from universal.
As of 2002, “An accurate estimate of the number of US veterinarians that aggressively treat pain in small animals is not currently available. Anecdotal evidence from talking with practitioners, new graduates, and students would suggest that the percentage is fairly low.”[v]
A study from 2006 found that 12% of veterinarians were still not using any analgesics for any surgery.[vi]
In a survey published in 2016, the vast majority (82%) of veterinarians provided just 3-7 days’ worth of pain medications for clients to give at home—even though a previous study demonstrated that cats were painful for at least 12 days post-op (the entire term of the study).[vii] Horrifyingly, 1.1% of practitioners do not give any pain meds at all, before, during or after surgery; and 6.6% of practices (163 individual clinics) do not send ANY pain control with clients to give to the cats at home.[viii]
It is important to note that this survey was conducted among members of the Veterinary Information Network, an online bulletin board and resource for vets. It costs a fair amount of money to belong to it. Only about 1/4 of practicing vets are members; and those who are, are the ones who are interested in keeping up with the profession, and in doing excellent medicine and surgery, according to modern practices. Unfortunately, a great many veterinarians fall far below this standard.
The real issue with declawing is pain.
Declawing is an excruciatingly painful orthopedic amputation; a radical surgical solution to a behavior problem. It is very rarely a medical problem (I’ve therapeutically declawed one cat in 22 years); in fact the AVMA and other professional organizations are definite in saying declawing has “no medical benefit” to the cat. In any case, the proposed ban provides an exemption for true medical conditions.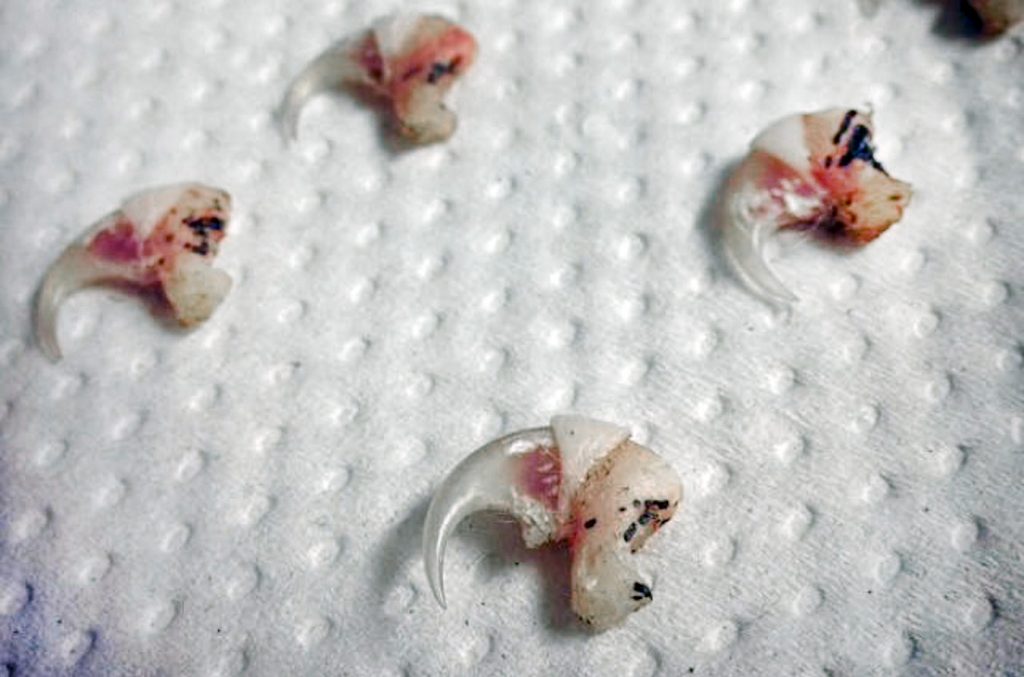 Laser declawed cat toes.
Laser declawed cat toes.
Declaw Complications
Veterinarians contend that, done properly, with adequate pain management, cats do just fine with having their toes amputated.
Many veterinarians feel that laser declawing is the least damaging declawing technique. Some vets who testify against declaw bans insist that laser is the standard, “everybody” is using it. Research, however, suggests that there is little if any difference in pain and long-term complications between laser and other techniques.[ix] [x]
A recent large survey of veterinarians found that 29% use guillotine nail trimmers; 70% use scalpel disarticulation; and only 36% use a laser.[xi]
Scalpel disarticulation, which uses a small, sharp scalpel to carve completely around the entire third phalanx (toe bone), causes more pain post-operatively than other techniques.[xii] [xiii] This is the most common declaw method.
Guillotine nail trimmers cause the most tissue damage, and may or may not leave part of the last phalanx (toe bone) in place. Whether that piece should or should not be removed has long been debated; different complications arise depending on the vet’s choice. If the little piece of bone is removed, tendon contracture may ensue; if the bone is left in, claw regrowth is quite common (<15%).[xiv]
Overall, complications of declawing surgery are very common. Studies put the rate of complications anywhere from 20% to over 80%.[xv] [xvi] [xvii] [xviii] Documented short- and long-term physical complications include:
- Pain
- Hemorrhage (bleeding)
- Lacerated paw pads
- Swelling
- Reluctance to bear weight on affected limbs
- Neuropraxia (transient motor paralysis)
- Radial nerve damage
- Lameness
- Infection
- Abscess
- Tissue necrosis
- Wound dehiscence (re-opening of surgical site)
- Incomplete healing
- Protrusion of 2nd phalanx (middle finger bone)
- Claw regrowth (can occur up to 15 years post-declaw)
- Scurs (growth of deformed claw segments)
- Retention of flexor process of 3rd phalanx
- Chronic draining tracts
- Self-mutilation
- Dermatitis
- Lethargy
- Palmigrade stance (walking on wrists)
- Chronic intermittent lameness
- Chronic pain syndrome
- Flexor tendon contracture
- Aggression
- Cystitis (bladder infection associated with stress
- Laser burns
On the effects of declawing, Professor Narda Robinson, Colorado State University, says, “The ensuing neuropathic pain and degenerative changes may plague [cats] for life.
Claw Regrowth
One common long-term complication of onychectomy is claw regrowth, with rates reportedly from 3.4% to 15.4%, depending on the study and the method of claw removal. A recent study found that claw regrowth was more common with use of a [guillotine] nail clipper than with use of a scalpel or laser (15.4% vs 6.5% and 3.4%); but claw regrowth occurred regardless of technique.[xix] This is the so-called “pebble in the shoe” issue. All the time that claw is growing—up to 15 years—it is causing pain.
Lameness
In one study, twelve cats (13.6%) were classified as mildly lame at the long-term recheck.[xx]
Another study found that lameness occurred more frequently in cats with [scalpel] disarticulation amputation (14/87, 16%) than in cats with bony amputation (4/80, 5%), possibly due to greater soft tissue trauma. Dehiscence (re-opening of incisions) occurred in 22% and 12% of cats, respectively.[xxi]
Other researchers documented that “43 cats showed lameness that persisted from 1-54 days. Long term follow up was done for 121/163 cats; one cat showed prolonged lameness (96 months).[xxii]
A study done at a university found “…there is an exceptionally high complication rate, 50% in the immediate postoperative period (during hospitalization period) and 19.8% in the late postoperative period (the period following hospital discharge).”
One case report’s authors suggest that tendon contracture, a long-known but newly-documented declaw complication, may have been seen previously but classified as “long-term” lameness.[xxiii]
A recent study of post-surgery problems also reported the highest rates of pain-related complications: up to 23% of cats with ongoing lameness, and 42.3% of cats showing signs of pain when their paws were handled. Owners also reported long-term behavioral changes in cats following declawing (house soiling); resistance to paws being handled; or increased incidence or severity of biting), compared with the same cats’ behavior before the procedure.[xxiv]
The newest study (2016) on medically unnecessary surgeries, concluded that there is clear evidence of pain and postoperative complications with declawing.[xxv]
“[T]he pain caused by this procedure often lasts long after the surgery is over. It can last the life of the cat, and even cause worse behavior problems than the one it supposedly set out to solve, destructive scratching, such as litter box avoidance and biting. After all, declawed cats come into animal shelters all the time, and are also trapped in feral cat colonies. – Dr. Marty Becker
Surgical Pain
Obviously, surgical incisions involve a significant amount of pain. Each incision hurts independently, so 10 incisions are far much more painful than just one. Orthopedic surgeries (those involving the musculoskeletal system) are particularly painful in humans. Declawing is an orthopedic surgery, and as one researcher states, “…orthopedic procedures involving the fingers and toes of humans are associated with severe postoperative pain….” [xxvi]
Incisions take 7-10 for initial healing. It takes about 6 months for an incision to completely heal, which is about how long it takes cats to settle into a new “normal” gait.[xxvii]
Neuropathic (Wind-Up) Pain
A different type of pain can occur when nerves are severed, as they are in a declaw procedure. According to Robin Downing, DVM, one of the foremost veterinary pain specialists in the world, “With nerve damage, there are changes that occur in the transmission of signals along the nerve fibers,” she explained. “The damaged nerves can set up a pain syndrome that is self-perpetuating. This means that the toes can become hypersensitive, or may even develop the sensations that humans with neuropathic pain experience.”[xxviii] Neuropathic, or maladaptive, pain results from damage to or dysfunction of the peripheral or central nervous system, rather than stimulation of pain receptors. The pain is out of proportion to the injury itself, and makes the central nervous system (brain and spinal cord) extra-sensitive. It originates in the nervous system itself, and is typically unresponsive to typical painkillers.[xxix] Different medications are required. Again, 10 (or 18) individual incisions greatly magnify the pain.
Pain Management
Many chronic declaw complications are attributable to inadequate analgesia before, during, and immediately after the surgery. The AVMA’s policy on declawing states, “Pain management is necessary (not elective) and required for this procedure. Multimodal pain management is recommended, and there should be a written aftercare plan.” Veterinarians’ perception and treatment of pain in animals has come a long way in the last 20 years, and even more in the last decade, but there is still a long way to go.
Unfortunately, this is an area where AVMA’s guidelines are commonly ignored. Cats’ own stoic nature makes this easy to do. It has long been acknowledged that pain in animals is difficult to assess, and cats take this opacity to the extreme.[xxx] [xxxi]
Pain management in animals is still in its infancy. Twenty years ago, giving pain medications for any condition, including surgery, was extremely uncommon. While the subject of pain has gotten a lot more attention in recent years, not all veterinarians acknowledge it or do anything about it.
Most troubling, perhaps, are the veterinarians who think declawing isn’t painfulat all, or that the pain is “trivial.” [xxxii] [xxxiii]
Nevertheless, declawing, like other orthopedic procedures, is more painful than other surgeries like spaying and neutering. The American Association of Feline Practitioners’ policy on declawing states:
“Physically, regardless of the method used, onychectomy (declawing) causes a higher level of pain than spays and neuters. Patients may experience both adaptive and maladaptive pain; in addition to inflammatory pain, there is the potential to develop long-term neuropathic or central pain if the pain is inadequately managed during the perioperative and healing periods.”
Pain management specialists emphasize the necessity of “effective, multi-modal peri-operative pain management” for pain of declawing—a procedure that has long served as the animal model for testing of analgesic effectiveness.[xxxiv] This view is trickling down through the ranks of everyday practitioners, but truly adequate analgesia for an appropriate amount of time appears to still be extremely rare.
A 2000 survey found that 30% gave no pain medication at all to cats undergoing declawing, while a large majority of the rest used butorphanol, which is poorly effective and short-acting (90 minutes-2 hours).[xxxv] [xxxvi] [xxxvii] [xxxviii]
A 2001 survey of Canadian vets found that 85% of pets received pre-op analgesics and 30-98% received post-op pain meds; but up to 12% of vets used no analgesia for any surgery.[xxxix]
A similar survey of U.S. vets, published around the same time, found that 30% of veterinarians used no pain meds at all for declawing; of those who did, 70% used primarily butorphanol (which was later determined to be effective for only 60-90 minutes, and completely inadequate for pain control in cats).[xl]
Still today, by their own admission, even the most conscientious veterinarians do not themselves provide adequate pain management. In a recent survey, the vast majority (82%) of veterinarians provided just 3-7 days’ worth of pain medications for clients to give at home[xli]—even though a previous study demonstrated that cats were painful for at least 12 days post-op (the entire term of the study).[xlii] Horrifyingly, 1.1% of practitioners do not give any pain meds at all, before, during or after surgery; and 6.6% of practices (163 individual clinics) do not send ANY pain control with clients to give to the cats at home.[xliii]
Even though these days most veterinarians say they use “opiates” for pain control, this may still mean only butorphanol, which is not much better than nothing at all.[xliv]
Chronic Pain 
There is actually such a thing as Chronic Pain Syndrome of Onychectomy. A noted veterinary pain specialist has found that “Feline patients who have had onychectomy (declaw) may experience chronic pain. Owners of such cats usually report one of several concerns, the most common of which is fear that the cat is still in pain, especially in the fore paws, because it seems to walk very lightly on those feet, as if walking on nails or glass. Another common concern is behavioral changes, which may include decreased activity, decreased appetite, or increased aggression. The inciting cause for these presentations within days to months to years is usually the lack of adequate acute pain control in the immediate postoperative period.[xlv] Yet the veterinary profession has yet to acknowledge the existence of such a syndrome.
Phantom Pain
An issue that has not been addressed by the veterinary profession is that of phantom pain. Of course, it’s impossible to know what cats are feeling with any certainty. But we know from human studies that 100% of amputees experience phantom sensations, and that about 80% of those sensations are painful. Some go away eventually, but most persist for years.
Cats have the same pain receptors, neural paths, and processing centers as humans or any other mammal. It is likely—virtually certain—that they also experience painful phantom sensations at least occasionally, and possibly for the rest of their lives. Multiply that by 10 (or 18 if all four paws are declawed) separate amputations, and that is why we believe that all declawed cats are painful at times, and some cats may be painful all the time.
Behaviorist Dr. Karen Overall has said, “There are also SA [sensory afferent] cells in the soft tissue at the bases of claws that signal the degree of extension and sideways displacement of the claw.[xlvi] This feature has been totally ignored when the subject of onychectomy [declawing] arises, yet certainly the presence of these cells could be one of the mechanisms for persistent discomfort of ‘phantom pain’ that some declawed cats appear to have. No population-specific prevalence data exist for this condition.”[xlvii]
Conclusion
To put these all this in perspective, there are, more or less, 80 million pet cats in the U.S. At least 20% are declawed (estimates range from 20-45%), which is 16,000,000 cats. If even only 5% have long-term painful complications (and the number is likely far higher), that’s still 800,000 cats with known chronic pain, obvious pain.
How many is too many to suffer?
Clearly, veterinarians as a profession have failed to keep up with modern medicine, failed to govern themselves, and failed to understand the universal, serious, and potentially lifetime pain they are causing cats by declawing. Sadly, there is no mechanism to enforce changes in the profession.
Therefore, legislation is necessary to stop the cruel and unnecessary practice of declawing.
Here is a rebuttal to the NJVMA’s spokesvet’s declawing testimony to the New Jersey Assembly Committee on Nov. 14, 2016 [button href=”https://citythekitty.org/rebuttal-to-njvmas-declawing-testimony/” color=”orange” newwindow=”yes”] The Truth About Declawing[/button]
References
[i] Benson GJ, Wheaton LG, Thurmon JC et al. Postoperative catecholamine response to onychectomy in isoflurane-anesthetized cats. Effect of analgesics. Veterinary Surgery. 1991;20:222-225
[ii] Cambridge AJ, Tobias KM, Newberry RC et al. Subjective and objective measurements of postoperative pain in cats. Journal of the American Veterinary Medical Association. 2000;217:685-690.
[iii] Smith JD, Allen SW, Quandt JE, et al. Indicators of postoperative pain in cats and correlation with clinical criteria. American Journal of Veterinary Research. 1996 Nov;57(11):1674-1678
[iv] Taylor PM, Robertson SA. Pain management in cats—past, present and future. Journal of Feline Medicine & Surgery. 2004;6:313-320.
[v] Hellyer PW. Treatment of pain in dogs and cats. Journal of the American Veterinary Medical Association. 2002 Jul 15;221(2):212-215.
[vi] Hewson J, Dohoo IR, Lemke KA. Perioperative use of analgesics in dogs and cats by Canadian veterinarians in 2001. Canadian Veterinary Journal. 2006 Apr;47:352-359.
[vii] Romans CW, Gordon WJ, Robinson DA, et al. Effect of postoperative analgesic protocol on limb function following onychectomy in cats. Journal of the American Veterinary Medical Association. 2005 Jul 1;227(1):89-93.
[viii] Ruch-Gallie R, Hellyer PW, Kogan LR. Survey of practices and perceptions regarding feline onychectomy among private practitioners. Journal of the American Veterinary Medical Association. 2016;249:291–298
[ix] Holmberg DL, Brisson BA. A prospective comparison of postoperative morbidity associated with the use of scalpel blades and lasers for onychectomy in cats. Canadian Veterinary Journal. 2006 Feb;47(2):162-3.
[x] Mison CB, Bohart GH, Walshaw R, et al. Use of carbon dioxide laser for onychectomy in cats. Journal of the American Veterinary Medical Association. 2002 Sep 1;221(5):651-3.
[xi] Ruch-Gallie R, Hellyer PW, Kogan LR. Survey of practices and perceptions regarding feline onychectomy among private practitioners. Journal of the American Veterinary Medical Association. 2016;249:291–298.
[xii] Martinez SA, Hauptmann J, Walshaw R. Comparing two techniques for onychectomy in cats and two adhesives for wound closure. Veterinary Medicine. 1993; 88:516-525.
[xiii] Clark K, Bailey T, Rist P, et al. Comparison of 3 methods of onychectomy. Canadian Veterinary Journal. 2014 Mar;55:255-262.
[xiv] Clark, ibid.
[xv] Ellison GW. Feline onychectomy complications: prevention & management. NAVC Clinician’s Brief. 2003 April:29-33.
[xvi] Tobias KS. Feline onychectomy at a teaching institution: a retrospective study of 163 cases. Veterinary Surgery. 1994; 23:274-280.
[xvii] Landsberg GM. Declawing is controversial but saves pets. A veterinarian survey. Veterinary Forum. 1991;8:66-67.
[xviii] Yeon SC, Flanders JA, Scarlett JM, et al. Attitudes of owners regarding tendonectomy and onychectomy in cats. J Am Vet Med Assoc. 2001;218:43-47.
[xix] Clark, ibid.
[xx] Clark, ibid.
[xxi] Martinez, op cit.
[xxii] Tobias KS. Feline onychectomy at a teaching institution: a retrospective study of 163 cases. Veterinary Surgery. 1994; 23:274-280.
[xxiii] Cooper MA, Laverty PH, Soiderer EE. Bilateral flexor tendon contracture following onychectomy in 2 cats. Canadian Veterinary Journal. 2005 Mar;46(3):244-6.
[xxiv] Clark K, Bailey T, Rist P, et al. Comparison of 3 methods of onychectomy. Canadian Veterinary Journal. 2014;55:255–262.
[xxv] Mills KE, von Keyserlingk MAG, Niel L. A review of medically unnecessary surgeries in dogs and cats. Journal of the American Veterinary Medical Association. 2016 Jan;248(2):162-171.
[xxvi] Benson GJ, Wheaton LG, Thurmon JC, et al. Postoperative catecholamine response to onychectomy in isoflurane-anesthetized cats: effect of analgesics. Veterinary Surgery. 1991;20(3):222-225.
[xxvii] Romans CW, Gordon WJ, Robinson DA, et al. Effect of postoperative analgesic protocol on limb function following onychectomy in cats. Journal of the American Veterinary Medical Association. 2005 Jul 1;227(1):89-93.
[xxviii] Becker M. The tragedy of post-declaw pain syndrome, and how to help cats who suffer from it. https://www.drmartybecker.com/veterinary-medicine/the-tragedy-of-post-declaw-pain-syndrome-and-how-to-help-cats-who-suffer-from-it/
[xxix] Lemke KA. Understanding the pathophysiology of perioperative pain
Canadian Veterinary Journal. 2004 May; 45(5): 405–413.
[xxx] Benson GJ, Wheaton LG, Thurmon JC et al. Postoperative catecholamine response todeclawing in isoflurane-anesthetized cats. Effect of analgesics. Veterinary Surgery. 1991;20:222-225.
[xxxi] Cambridge AJ, Tobias KM, Newberry RC et al. Subjective and objective measurements of postoperative pain in cats. Journal of the American Veterinary Medical Association. 2000;217:685-690.
[xxxii] Curcio K, Bidwell LA, Bohart GV, et al. Evaluation of signs of postoperative pain and complications after forelimb onychectomy in cats receiving buprenorphine alone or with bupivacaine administered as a four-point regional nerve block. Journal of the American Veterinary Medical Association. 2006 Jan 1;228(1):65-8.
[xxxiii] Ruch-Gallie, op cit.
[xxxiv] Hellyer P, et al. AAHA/AAFP pain management guidelines for dogs and cats. Journal of Feline Medicine and Surgery. 2007;9:466-480.
[xxxv] Wagner AE, Hellyer PW. Survey of anesthesia techniques and concerns in private veterinary practice. Journal of the American Veterinary Medical Association. 2000 Dec 1;217(11):1652-1657.
[xxxvi] Lascelles BD, Robertson SA. Use of thermal threshold response to evaluate the antinociceptive effects of butorphanol in cats. American Journal of Veterinary Research. 2004;65:1085–1089.
[xxxvii] Gordon WJ, Romans C, Evans R, et al. Objective evaluation of the efficacy of bupivacaine, butorphanol, and fentanyl patch after onychectomy using pressure platform gait analysis (abst), in Proceedings. 31st Annual Conference of the Veterinary Orthopedic Society, 2004.
[xxxviii] Robertson SA, Taylor PM, Lascelles BDX, et al. Changes in thermal threshold response in eight cats after administration of buprenorphine, butorphanol and morphine. Veterinary Record. 2003;153:462-465.
[xxxix] Hewson J, Dohoo IR, Lemke KA. Perioperative use of analgesics in dogs and cats by Canadian veterinarians in 2001. Canadian Veterinary Journal. 2006 Apr;47:352-359.
[xl] Wagner AE, Hellyer PW. Survey of anesthesia techniques and concerns in private veterinary practice. Journal of the American Veterinary Medical Association. 2000 Dec 1;217(11):1652-1657.
[xli] Ruch-Gallie, op cit.
[xlii] Romans CW, Gordon WJ, Robinson DA, et al. Effect of postoperative analgesic protocol on limb function following onychectomy in cats. Journal of the American Veterinary Medical Association. 2005 Jul 1;227(1):89-93.
[xliii] Ruch-Gallie, op cit.
[xliv] Ruch-Gallie, op cit.
[xlv] Gaynor JS. Chronic pain syndrome feline onychectomy. NAVC Clinician’s Brief. April 2005.
[xlvi] Gordon G, Jukes MG. Dual organization of the exteroceptive components of the cat’s gracile nucleus. Journal of Physiology. 1964 Sep;173:263-90.
[xlvii] Overall K. Clinical Behavior Medicine for Small Animals. 1997. St. Louis, MO: Mosby, Inc.
